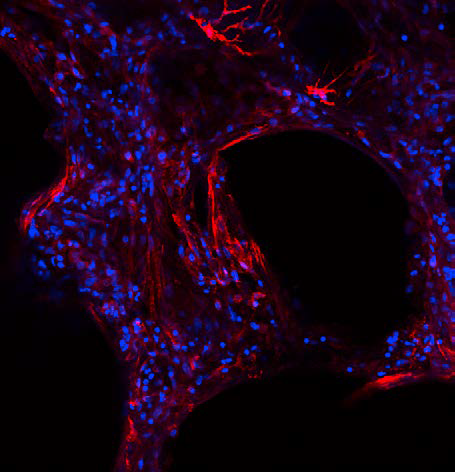
Pulmonary fibrosis (PF) comprises a spectrum of rapidly progressive lung diseases that are mainly characterized by aberrant wound healing processes leading to uncontrolled deposition of extracellular matrix (ECM) proteins and consequent destruction of lung architecture. The underlying mechanisms are not yet fully understood. In the context of the COVID-19 pandemic, it has been reported that a large number of patients who had recovered from their acute COVID-19 pneumonia develop advanced PF or post-COVID interstitial lung disease (PC-ILD), highlighting the importance of identifying new biomarkers for distinct PF diseases. Together with several industry partners, Fraunhofer ITEM scientists published novel data on neoepitope biomarkers of type I, III and VI collagen formation or degradation in precision-cut lung slices (PCLS) from patients with PF (Hesse et al., 2022), with a focus on the treatment effects of antifibrotic drugs. They found that PRO-C3 and C3M were modulated by nintedanib, suggesting that nintedanib exerts antifibrotic effects via type III collagen remodeling. Linking the study to clinical data showed C3M to be a promising biomarker of response to treatment with nintedanib. This study has once again highlighted the use of PCLS as a highly translational model to study the underlying mechanisms of pulmonary fibrosis and to advance preclinical drug development and clinical decision-making.
 Fraunhofer Institute for Toxicology and Experimental Medicine
Fraunhofer Institute for Toxicology and Experimental Medicine